I have seen patients lose a limb over a wound the size of a dime — not because they ignored it, but because they never felt it in the first place.
This is one of the most important things I can say to any diabetic patient or their family: the absence of pain does not mean the absence of a problem. Diabetic peripheral neuropathy means that a wound can develop, worsen, become infected, and begin threatening the underlying bone without the patient ever feeling anything significant enough to prompt concern.
A diabetic foot ulcer can become a medical emergency faster than most patients realize — and I have seen patients lose a limb over a wound the size of a dime, not because they ignored it, but because they never felt it.
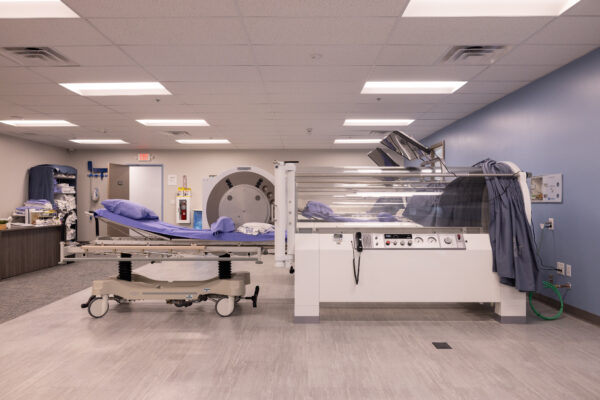
My name is Dr. Cyrus Garmo. I am board-certified in Internal Medicine and certified in Hyperbaric Medicine through ATMO, recognized by the Undersea and Hyperbaric Medical Society. At RevitalizeMe Hyperbaric Oxygen and Wound Care in Saginaw, Michigan, preventing amputation is one of the central reasons we exist. I want to walk through how a diabetic foot ulcer develops, how quickly it can become serious, and what appropriate care looks like.
In this article:
- Why diabetics often do not feel their foot wounds
- How a small wound becomes a serious infection in days
- The path from ulcer to osteomyelitis to amputation
- How to check your feet and what to look for
- What proper wound care involves
- When hyperbaric oxygen therapy becomes part of the plan
Why Diabetics Often Do Not Feel Their Foot Wounds
Diabetes damages nerves throughout the body, but peripheral neuropathy affecting the feet and lower legs is one of the most clinically consequential complications. Patients lose the ability to feel pressure, temperature, and pain in the affected areas. The protective sensation that would normally alert you that something is wrong is simply not there.
A shoe that rubs in the wrong place. A small stone inside a sock. A blister that forms and breaks. Under normal circumstances any of these would be uncomfortable enough to prompt attention. For a patient with significant diabetic neuropathy, they may go completely unnoticed.
This is why daily foot inspection is one of the most important habits a diabetic patient can develop. Not because inspecting your feet will prevent neuropathy, but because your eyes can catch what your nerves can no longer report.
How a Small Wound Becomes a Serious Infection in Days
Diabetes does not only affect nerve sensation. It impairs virtually every mechanism involved in wound healing and infection defense.
Elevated blood glucose creates an environment that supports bacterial growth. Vascular disease — also more common in diabetic patients — reduces blood flow to the lower extremities, which means less oxygen, fewer immune cells, and slower healing. White blood cell function is impaired in poorly controlled diabetes, reducing the body’s ability to fight infection effectively.
Put these factors together and you have a situation where a small wound that might heal quickly in a healthy person becomes a wound that does not close, gets colonized by bacteria, and can progress to serious soft tissue infection within days.
I have seen patients present to our center over a weekend with a wound that their family noticed on Friday that was already showing signs of deep tissue involvement by Monday. This is not a slow, predictable process in a diabetic patient with vascular compromise. It can move fast.
The Path from Foot Ulcer to Osteomyelitis to Amputation
An open wound on a diabetic foot is an entry point for bacteria. Surface infection that is not adequately treated can progress to deeper soft tissue involvement. From there, infection can reach the bone.
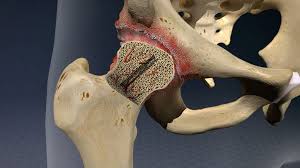
Osteomyelitis — bone infection — is one of the most serious complications of diabetic foot ulcers. Once infection is established in bone, treatment becomes significantly more complex. Bone has limited blood supply relative to soft tissue, which means antibiotics have a harder time reaching the infection and the immune response is less effective.
In cases where infection is extensive or the tissue is no longer viable, amputation may become the safest option to prevent the spread of infection and protect the patient’s life. This outcome is preventable in many cases with early recognition and appropriate treatment. That is the whole point.
How to Check Your Feet — and What to Look For
If you are a diabetic patient, checking your feet daily is something your physician has likely told you. I want to be specific about what that means in practice.
Use good lighting. Look at the top, bottom, sides, and between every toe. If you cannot see the bottom of your feet comfortably, use a mirror or ask a family member to help. Look for anything that was not there before — any break in the skin, any redness, any area that looks different in color or texture, any swelling, any drainage.
Also notice whether any area feels warmer than the surrounding tissue when you touch it. Warmth can indicate inflammation or early infection even before a visible wound develops.
Do not assume that no pain means no problem. That assumption is specifically what this disease takes advantage of. If you find anything that concerns you, contact your physician or wound care specialist the same day.
If you are a diabetic patient with a foot wound that is not healing, or a family member concerned about a loved one, contact RevitalizeMe Hyperbaric Oxygen and Wound Care in Saginaw. Call (989) 320-4434 or visit revitalizemehyperbaricwoundcare.com. We work with your existing care team and accept Medicare, Medicaid, and most major private insurance.
Schedule a ConsultationWhat Proper Wound Care Involves
Diabetic foot ulcer care is not simply a matter of covering the wound and waiting. Effective treatment addresses the wound itself and the factors driving it.
Debridement — the removal of dead or devitalized tissue — is a core component. Dead tissue creates a barrier to healing and a breeding ground for bacteria. Offloading is another critical element. Continued pressure on a wound from walking or ill-fitting footwear prevents healing regardless of what dressings are applied.
Infection management, vascular assessment, glycemic optimization, and nutritional evaluation are all part of a comprehensive approach. The wound cannot be managed in isolation from the patient’s overall medical picture.
When Hyperbaric Oxygen Therapy Becomes Part of the Plan
For diabetic foot ulcers that are Wagner Grade 3 or higher and have not shown adequate response to 30 days of standard wound care, hyperbaric oxygen therapy is a covered Medicare indication under National Coverage Determination 20.29.
Wagner Grade 3 means the ulcer has penetrated to deep tissue — tendon, joint capsule, or bone — or involves abscess or osteomyelitis. These are the wounds where tissue hypoxia is a significant driver of non-healing and where HBOT’s mechanism of dramatically increasing oxygen delivery to compromised tissue is directly relevant.
At our center, HBOT for diabetic foot ulcers is delivered in coordination with our comprehensive wound care program. It is one component of a plan that addresses the wound, the vascular situation, the infection status, and the patient’s overall medical management.
For referring providers and podiatrists: if you have a patient with a Wagner Grade 3 or higher diabetic foot ulcer that has not responded to 30 days of standard care, HBOT authorization can be pursued through Medicare. We handle the prior authorization process and work directly with your team. Call us at (989) 320-4434.
Schedule a ConsultationFAQ: Diabetic Foot Ulcers
How fast can a diabetic foot ulcer become infected?
In a diabetic patient with neuropathy and vascular compromise, a wound can progress from a surface break to serious infection relatively quickly — sometimes within days. If you notice a new wound on your foot, contact your physician the same day rather than waiting.
What does a diabetic foot ulcer look like?
A diabetic foot ulcer typically appears as a break in the skin, often on the bottom of the foot, the heel, or over a bony prominence. There may or may not be drainage. Surrounding redness, warmth, or swelling may indicate infection. If you are uncertain whether what you are seeing requires attention, contact your physician.
Does Medicare cover wound care for diabetic foot ulcers?
Medicare covers wound care services and, for qualifying ulcers — Wagner Grade 3 or higher that have not responded to 30 days of standard care — hyperbaric oxygen therapy under NCD 20.29. Our team verifies coverage and handles authorization before treatment begins.
How do I know if my foot wound is serious?
Any open wound on a diabetic foot should be evaluated by a physician or wound care specialist promptly. Do not attempt to determine severity based on pain level — neuropathy means pain is not a reliable indicator. Signs that warrant urgent evaluation include any wound that is not improving, surrounding redness or warmth, drainage that is cloudy or has an odor, or darkening of the tissue. When in doubt, call your physician the same day.
Can a diabetic foot ulcer lead to amputation?
Yes, in cases where infection progresses to osteomyelitis or the tissue is no longer viable, amputation may become necessary to protect the patient’s life. This outcome is preventable in many cases with early recognition and appropriate treatment. Preventing amputation is one of the primary goals of diabetic wound care and HBOT when clinically indicated.
— Dr. Cyrus Garmo, MD
Board-Certified Internal Medicine | Certified Hyperbaric Medicine, ATMO/UHMS
RevitalizeMe Hyperbaric Oxygen and Wound Care, Saginaw, MI
Individual results vary. This article is for informational purposes only and does not constitute medical advice. Please consult your physician regarding your individual care.