The most common reason patients wait months longer than they should to call our center is not that they do not want treatment — it is that they are not sure Medicare will cover it and they do not want to find out the hard way.
I hear this every week. A patient or their family member has been dealing with a non-healing wound, a radiation injury, or another condition for months. They have heard about hyperbaric oxygen therapy. They want to explore it. But the insurance question stops them before they ever pick up the phone.
My name is Dr. Cyrus Garmo. I am board-certified in Internal Medicine and certified in Hyperbaric Medicine through ATMO, recognized by the Undersea and Hyperbaric Medical Society. At RevitalizeMe Hyperbaric Oxygen and Wound Care in Saginaw, Michigan, we handle insurance verification and prior authorization for every patient before treatment begins. I want to answer the coverage question directly so it is no longer the thing standing between you and getting the care you need.
In this article:
- Why insurance coverage is the question we get asked most
- What Medicare NCD 20.29 actually says
- Which conditions Medicare covers for HBOT — the complete list
- What Medicare does not cover and what that means for you
- What Medicaid and private insurance cover
- How the authorization process works at RevitalizeMe
- What if my condition is not on the Medicare list
Why Insurance Coverage Is the Question We Get Asked Most
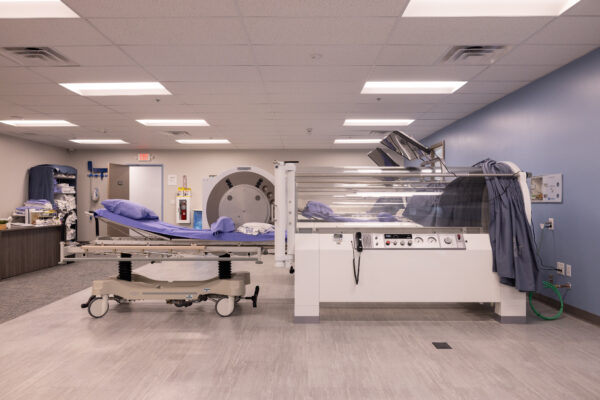
Hyperbaric oxygen therapy has a reputation — sometimes deserved, sometimes not — for being expensive and hard to access. Part of that reputation comes from the wellness industry, where soft-sided hyperbaric chambers are marketed directly to consumers at significant out-of-pocket cost for conditions that are not clinically recognized indications.
Medical-grade hyperbaric oxygen therapy at a physician-supervised center is a different conversation entirely. For the conditions Medicare recognizes, coverage exists and has existed for decades. The problem is that most patients do not know which conditions are on that list, and most do not realize that a center like ours handles the entire authorization process on their behalf.
The short answer to the question is this: yes, Medicare covers hyperbaric oxygen therapy for specific conditions. If your condition is on the list, the process of getting authorized is something we manage for you. If you are not sure whether your condition qualifies, a consultation is the right starting point and we can tell you where you stand before anything moves forward.
What Medicare NCD 20.29 Actually Says
Medicare’s coverage for hyperbaric oxygen therapy is governed by National Coverage Determination 20.29. This is the formal policy document that defines which conditions qualify for coverage, under what circumstances, and what documentation requirements apply.
NCD 20.29 divides HBOT coverage into two categories. The first category covers conditions where HBOT is the primary treatment — situations like decompression sickness and arterial gas embolism where hyperbaric oxygen is the established standard of care. The second category covers conditions where HBOT is used as an adjunctive treatment alongside other therapies — situations like diabetic foot ulcers and delayed radiation injuries where HBOT complements the primary wound care or medical management plan.
Both categories require physician prescription and supervision. At a properly run center, every patient receiving Medicare-covered HBOT has a treating physician overseeing their care, documented medical necessity, and a treatment plan that meets the specific criteria Medicare requires for the relevant indication.
The documentation requirements matter. Medicare does not simply cover HBOT because a patient has a qualifying diagnosis. The medical record has to demonstrate that the specific criteria for that indication are met. This is where working with an experienced hyperbaric center makes a significant difference — we know what Medicare needs to see and we build the documentation correctly from the beginning.
Which Conditions Medicare Covers for HBOT — The Complete List
Here is every condition currently covered under Medicare NCD 20.29 for hyperbaric oxygen therapy:
Acute carbon monoxide intoxication. Carbon monoxide poisoning is one of the clearest indications for HBOT. High-concentration oxygen delivered under pressure rapidly displaces carbon monoxide from hemoglobin and is the standard of care for significant exposures.
Decompression illness. Also known as decompression sickness or the bends, this condition affects divers and others exposed to rapid pressure changes. HBOT is the definitive treatment.
Gas embolism. Air or gas bubbles that enter the bloodstream — a serious and potentially life-threatening condition — are treated with hyperbaric oxygen to reduce bubble size and support tissue oxygenation.
Crush injuries, suturing of severed limbs, and other acute traumatic peripheral ischemia. When tissue is severely injured and blood supply is compromised, HBOT can support tissue survival during the critical period of recovery.
Progressive necrotizing infections — necrotizing fasciitis. These are aggressive, rapidly spreading soft tissue infections. HBOT is used alongside surgical management to support tissue and reduce the spread of infection.
Acute peripheral arterial insufficiency. When arterial blood supply to a limb is acutely compromised, HBOT can support tissue oxygenation while the underlying vascular issue is addressed.
Preparation and preservation of compromised skin grafts and flaps. For skin grafts or tissue flaps that are at risk of failure due to compromised blood supply, HBOT supports tissue survival and healing. This is a covered Medicare indication with strong clinical evidence.
Chronic refractory osteomyelitis. Bone infections that have not responded to standard antibiotic therapy and surgical management qualify for HBOT coverage. The elevated oxygen environment supports immune function and antibiotic effectiveness in infected bone tissue.
Osteoradionecrosis as an adjunct to conventional treatment. Radiation damage to bone — most commonly the jaw following head and neck radiation — is a covered indication. HBOT promotes new blood vessel formation in radiation-damaged bone and supports healing.
Soft tissue radionecrosis as an adjunct to conventional treatment. Delayed radiation injury to soft tissue — including radiation cystitis following pelvic radiation and radiation proctitis — is covered under this indication. This is one of the conditions where HBOT has the strongest clinical evidence base.
Cyanide poisoning. HBOT is used in the management of significant cyanide poisoning as part of emergency treatment.
Actinomycosis. A specific type of bacterial infection that is difficult to treat with antibiotics alone. HBOT is covered as an adjunct to standard antibiotic therapy for appropriate cases.
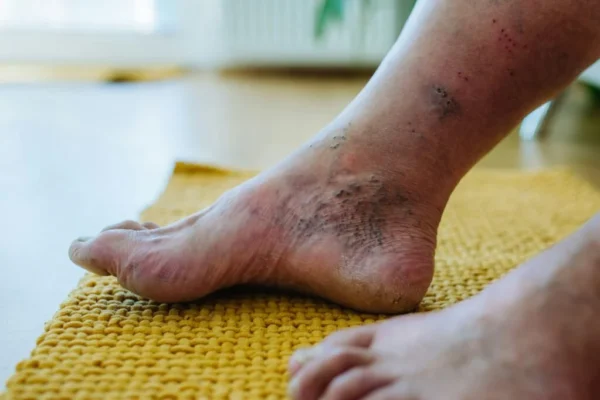
Diabetic wounds of the lower extremity. This is the indication most relevant to the patients we see most often. Medicare covers HBOT for diabetic patients with lower extremity wounds that meet all of the following criteria: the patient has type 1 or type 2 diabetes; the wound is Wagner Grade III or higher; the patient has failed an adequate course of standard wound therapy; and the treating physician has evaluated the wound and determined that there are no other treatable causes of failure to heal.
That last indication — diabetic wounds of the lower extremity — is the one I want to spend a moment on because the criteria matter and patients sometimes hear a simplified version that leads to confusion later.
Wagner Grade III means the ulcer has penetrated to deep tissue — tendon, joint capsule, or bone — or involves abscess or osteomyelitis. It is not a superficial wound. And the requirement for failure of standard wound therapy means the patient must have received appropriate wound care for 30 days without adequate healing progress before HBOT authorization is pursued. These criteria exist because they define the patient population where the evidence for HBOT benefit is strongest. They are also criteria that our team evaluates carefully during the intake process so we can tell you clearly whether your wound meets them.
If you have a diabetic wound and you are wondering whether you qualify, call us at (989) 320-4434 or visit revitalizemehyperbaricwoundcare.com. We will review your situation and tell you where you stand before anything moves forward.
Schedule a ConsultationWhat Medicare Does Not Cover — and What That Means for You
I want to be straightforward about this because patients deserve a clear answer.
Medicare does not cover HBOT for conditions outside of NCD 20.29. This includes a number of conditions that the Undersea and Hyperbaric Medical Society has recognized as having clinical evidence for HBOT benefit — conditions like sudden sensorineural hearing loss, avascular necrosis, and certain other indications — but that Medicare has not included in its coverage determination.
For those conditions, Medicare coverage is not available. However, many private insurance plans do cover UHMS-recognized indications even when Medicare does not. And for some patients, self-pay options are available depending on the clinical situation and the treatment being considered.
The most important thing is not to assume you are not covered without actually checking. Coverage determinations are specific to your individual plan, your diagnosis, and the documentation supporting medical necessity. We verify that for every patient before treatment begins. Do not let an assumption about coverage stop you from having a conversation.
What Medicaid and Private Insurance Cover
Medicaid coverage for HBOT varies by state. In Michigan, Medicaid generally follows Medicare coverage standards for HBOT indications, which means the conditions listed under NCD 20.29 are typically covered for Medicaid patients as well. Our team verifies Medicaid coverage for each patient individually before treatment begins.
Private insurance coverage is more variable. Most major private insurance plans cover the Medicare-recognized indications. Many also cover UHMS-recognized indications that Medicare does not — conditions like sudden sensorineural hearing loss and avascular necrosis — particularly when UHMS recognition is documented and medical necessity is clearly established.
We accept Medicare, Medicaid, and most major private insurance plans at RevitalizeMe. We are also actively credentialing with Tricare and the VA. If you are not sure whether your specific plan covers the treatment you are considering, call us at (989) 320-4434 and we will look into it with you.
Schedule a ConsultationIf you have been told your condition qualifies for HBOT and you want to understand your coverage before scheduling, contact RevitalizeMe Hyperbaric Oxygen and Wound Care in Saginaw. Call (989) 320-4434 or visit revitalizemehyperbaricwoundcare.com. We verify coverage before treatment begins — no surprises.
Schedule a ConsultationHow the Authorization Process Works at RevitalizeMe
This is the part that most patients do not realize — you do not have to navigate the authorization process on your own. We handle it.
Here is how it works from the moment you contact us.
First, we do an initial intake review. You call us or fill out a consultation request. We gather basic information about your diagnosis, your current treatment history, and your insurance. This gives us what we need to do a preliminary assessment of whether your situation is likely to qualify for coverage.
Second, we schedule a consultation. You come in and I evaluate you directly. We review your medical records, assess your wound or condition, and determine whether HBOT is clinically appropriate for your situation. If it is, we document the medical necessity in the way Medicare and your insurer need to see it.
Third, we handle prior authorization. For Medicare and most private insurance plans, HBOT requires prior authorization before treatment begins. Our team submits that authorization with the supporting clinical documentation. We communicate with your insurer directly. We follow up. We manage that process so you do not have to.
Fourth, we coordinate with your referring providers. We communicate back to your primary care physician, your wound care team, your specialist — whoever is involved in your care — so everyone is aligned on the treatment plan.
Fifth, treatment begins. Once authorization is in place and everyone is aligned, we schedule your first session and walk you through exactly what to expect.
From the time a patient calls us to the time treatment begins varies depending on the complexity of the authorization and how quickly records come together. We work to move as efficiently as possible, especially for time-sensitive situations. If you have an urgent clinical situation, tell us when you call and we will prioritize accordingly.
What If My Condition Is Not on the Medicare List?
This is a question I want to answer carefully because the answer matters for a lot of patients.
If your condition is not covered under Medicare NCD 20.29, Medicare will not pay for HBOT regardless of how medically appropriate it may be for your situation. That is a real limitation and I am not going to minimize it.
However, not being covered by Medicare does not automatically mean HBOT is out of reach. Here are the options worth exploring:
Private insurance may cover it. Many private plans cover UHMS-recognized indications that Medicare does not. Your plan documents and a direct conversation with your insurer — or with our team — can clarify this quickly.
A consultation is still the right first step. Come in, let us evaluate your situation, and we will give you a clear picture of what your options are. We will not recommend treatment we cannot support clinically and we will not leave you without a clear understanding of what coverage looks like for your specific situation.
The worst outcome is a patient who needed care and never called because they assumed they were not covered. That assumption is worth testing with a phone call.
Call us at (989) 320-4434 or visit revitalizemehyperbaricwoundcare.com. We accept Medicare, Medicaid, and most major private insurance. If you are not sure where you stand, that is exactly what a consultation is for.
Schedule a ConsultationFAQ: Medicare Coverage for Hyperbaric Oxygen Therapy
Does Medicare pay for hyperbaric oxygen therapy?
Yes, Medicare covers hyperbaric oxygen therapy for specific conditions listed under National Coverage Determination 20.29. Covered conditions include diabetic foot ulcers meeting specific criteria, delayed radiation injuries, chronic refractory osteomyelitis, compromised skin grafts and flaps, and several other indications. Coverage requires physician prescription, documented medical necessity, and prior authorization. Contact our center at (989) 320-4434 to find out whether your specific situation qualifies.
Schedule a ConsultationWhat conditions qualify for Medicare HBOT coverage?
The conditions covered under Medicare NCD 20.29 include diabetic wounds of the lower extremity meeting Wagner Grade III or higher criteria, soft tissue radionecrosis, osteoradionecrosis, chronic refractory osteomyelitis, compromised skin grafts and flaps, necrotizing soft tissue infections, acute peripheral arterial insufficiency, crush injuries and acute traumatic ischemia, decompression illness, gas embolism, carbon monoxide poisoning, cyanide poisoning, and actinomycosis. Each indication has specific criteria that must be documented in the medical record.
Do I need a referral for Medicare to cover hyperbaric oxygen therapy?
You do not necessarily need a formal referral to contact our center or schedule a consultation. However, Medicare coverage for HBOT requires physician prescription and documented medical necessity. We coordinate directly with your existing care team and can work with your primary care physician or specialist to establish the documentation Medicare requires. Call us and we will walk you through the process.
Does Medicare Advantage cover hyperbaric oxygen therapy?
Medicare Advantage plans are required to cover at minimum everything that traditional Medicare covers, which includes the HBOT indications under NCD 20.29. Some Medicare Advantage plans may have additional prior authorization requirements or network restrictions. Our team verifies coverage for Medicare Advantage patients individually before treatment begins. Call us at (989) 320-4434 with your plan information and we will check your specific coverage.
Schedule a ConsultationWhat does hyperbaric oxygen therapy cost without insurance?
The cost of HBOT without insurance coverage varies by center and by the number of sessions required for the specific indication being treated. Rather than publish a number that may not reflect your individual situation, I would encourage you to call us directly at (989) 320-4434. We will review your insurance coverage first — because in many cases patients who assume they are not covered actually are — and if self-pay is the relevant option for your situation we will discuss that with you directly and transparently.
Schedule a Consultation— Dr. Cyrus Garmo, MD
Board-Certified Internal Medicine | Certified Hyperbaric Medicine, ATMO/UHMS
RevitalizeMe Hyperbaric Oxygen and Wound Care, Saginaw, MI
Individual results vary. This article is for informational purposes only and does not constitute medical advice. Please consult your physician regarding your individual care.